Editor’s note: The following article is an op-ed, and the views expressed are the author’s own. Read more opinions on theGrio.
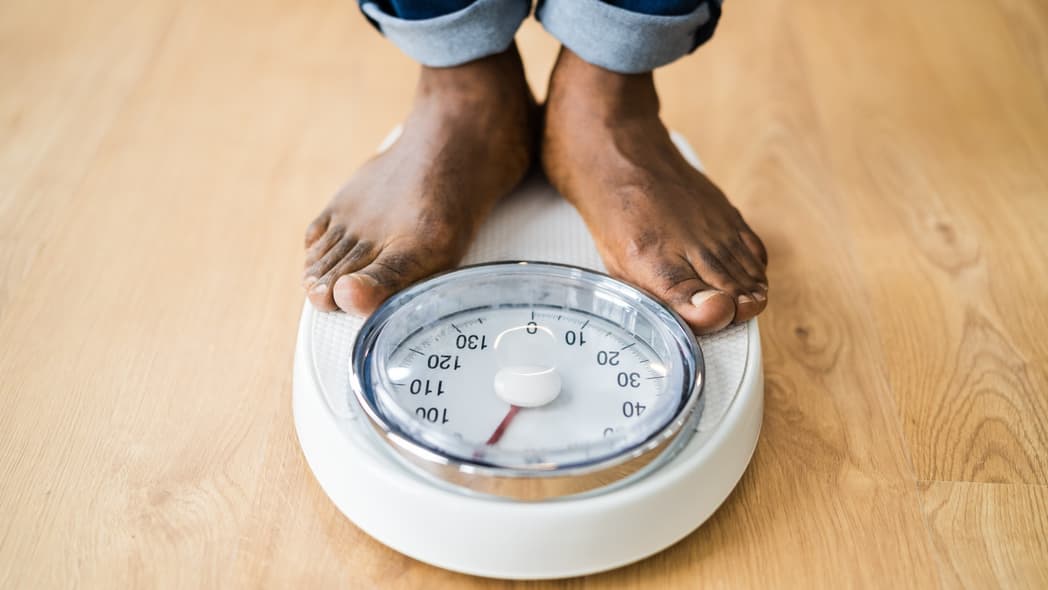
Today, nearly 108 million American adults are living with obesity, and that number is expected to jump significantly, crossing the 50% threshold by 2030. While that statistic is undoubtedly chilling, for Black Americans 2030 has already arrived.
Obesity is more prevalent in the Black community than in any other demographic group in the United States. Sadly, 49.9% of non-Hispanic Black adults live with obesity. For Black women, the obesity epidemic is worse: approximately four out of every five Black women are living with overweight/obesity, the highest rate of any group in the U.S.
As a physician and the incoming president of the National Medical Association (NMA) — the nation’s largest medical association fighting for parity and justice in medicine and the elimination of health disparities in the Black community — I believe that addressing the obesity epidemic in the Black community has never been more urgent. And I believe that if we don’t take swift action to address and uplift the health of Black Americans — including ensuring access to critical, lifesaving medical treatments — we’ll lose an opportunity to reverse the consequences of obesity for millions of Black Americans. And those consequences are catastrophic.
Obesity exacerbates a myriad of other health conditions, including Alzheimer’s, infant mortality, multiple cancers, limb amputations and the most troubling of the coexisting conditions of obesity, cardiovascular disease and type 2 diabetes — of which 36.4 million Americans were living in 2021. Black adults are not only twice as likely as white adults to have obesity and develop this disorder, but Black Americans consistently experience strikingly higher morbidity and mortality burdens of cardiovascular disease — and are more than twice as likely to die of the disease than white adults.
For Black Americans, the public health challenges of obesity are further compounded by systemic hurdles we regularly face in accessing health care. The Black community’s journey towards health equity faces many upstream social determinants and personal barriers that lie far beyond the doctor’s office. But one of the most important battles is ensuring that Black Americans have equitable access to the comprehensive continuum of treatment and care options.
Effective obesity treatment requires physicians to custom-tailor treatments that pull from a menu of treatment options — which could include healthier diets and daily exercise, surgery, and anti-obesity medications (AOMs). While no single treatment is a silver bullet, FDA-approved AOMs are quickly showing that the fight against obesity is winnable.
But for Black Americans, the fight doesn’t end there.
Health
Despite obesity being a treatable disease, Medicare prescription policies are still creating hurdles for many Black chronically and catastrophically ill patients. Outdated regulations under Medicare prevent many Black seniors from accessing these new life-saving medications, despite CDC reports showing that 40% of adults aged 60 and older and over 41% of people with disability are living with obesity. These Black recipients rely on Medicare for their primary health insurance coverage and depend on it for access to these vital obesity treatment options.
Legislative bills have been introduced on Capitol Hill in both the U.S. House and Senate but have not been enacted. One critical bill including the Treat and Reduce Obesity Act (TROA), which would grant Medicare recipients access to AOMs through Medicare Part D, has remained halted for a decade while obesity rates climb nationwide. Black Americans are paying the price with their lives. Congress, you have an opportunity to make a big difference here by passing this legislation.
Other federal insurers including the Veterans Administration, Department of Defense, Indian Health Service and the Office of Personnel Management offer AOM coverage for their beneficiaries and their families. Only our seniors, people with disabilities or chronically and catastrophically ill patients, — many of whom are Black Medicare beneficiaries — are left without equitable access to these game-changing metabolic therapies.
It is time to advocate for legislative changes that will ensure every individual has access to these life-saving medical treatments for obesity. In 2019, the estimated annual medical cost of obesity in the U.S. was $173 billion. Medical costs for adults with obesity were $1,861 higher than those not living with the disease.
For millions of Americans — and especially Black Americans shouldering the greatest burden of the obesity epidemic — we cannot afford to wait any longer.
Prevention is important. While these drugs are never a replacement for good nutrition and adequate physical activity, it’s time to finally address the growing obesity epidemic by ensuring that those living with obesity have access to every tool in the physician’s toolbox — including AOMs. These medications, when used in conjunction with lifestyle and behavioral modifications, can significantly improve health outcomes and enhance the quality of life for individuals living with obesity.
For Black Americans living with obesity, we are morally obligated as a society to collectively demand that the obesity policy is updated to ensure health equity is not just an aspiration but a reality.

Virginia A. Caine, M.D., is the Director and Chief Medical Officer of the Marion County Public Health Department in Indianapolis, Indiana. She served as Chair of the Board of Trustees for the NMA, is currently Chair of the Internal Medicine Infectious Diseases and Co-Chair HIV Sections, as well as the upcoming 125th NMA President. She is a past President of the American Public Health Association and co-chair of Jump IN for Healthy Kids.